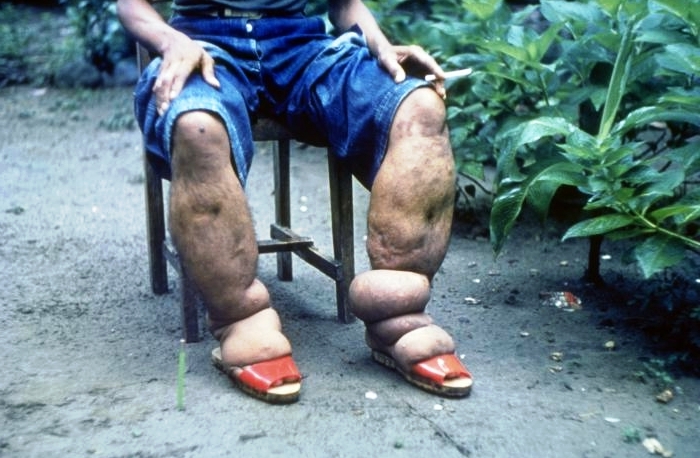
Lymphatic Filariasis
A Disease of Body Deformities in Tropical and Sub-tropical Regions of the World
-Dr. Arvind Singh
Lymphatic filariasis which also known as Elephantiasis is an infectious disease caused by thread-like worms and is globally considered as Neglected Tropical Disease. Neglected Tropical Diseases are those which almost exclusively affect impoverished people living in rural areas or poor urban slums of low-income countries. They are caused by parasitic worms, bacteria, and protozoa. They can be fatal but they primarily cause chronic lifelong disabilities leading to disfigurement, impaired child development, poor pregnancy outcomes, and impaired worker productivity.
Victims of neglected tropical diseases also encounter serious stigma in their communities, adding social consequences to their health problems. As a result, neglected tropical diseases affect the health of poor populations, and they mire infected individuals in poverty. On national and regional scales, their effects are so dire that these diseases are considered a condition that promotes and perpetuate poverty.
Lymphatic filariasis is a serious health problem found mainly in tropical and sub-tropical regions of the world. About 1.4 billion people in 73 countries of the world are threatened by the disease. Nearly 80% of these people live in the countries of Bangladesh, Democratic Republic of Congo, Ethiopia, India, Indonesia, Myanmar, Nigeria, Nepal, Philippines and the United Republic of Tanzania. Furthermore, more than 120 million are currently infected, with about 40 million disfigured and incapacitated by the disease. Lymphatic filariasis afflicts over 25 million men with the genital disease and over 15 million with lymphoedema (swelling). Lymphatic filariasis is thought to have affected humans since approximately 4000 years ago.
What are the different types of Filariasis?
Filariasis is categorized into three types on the basis of niche occupation by filarial nematodes within the human body. These include lymphatic filariasis, subcutaneous filariasis, and serous cavity filariasis.
In lymphatic filariasis, the worms inhabit the lymphatic system, including the lymph nodes. It is the most common type of filariasis.
Subcutaneous filariasis is caused by Loa loa, Mansonella streptocera, and Orchocerca volvulus. These worms inhabit the subcutaneous layer of skin, in the fat layer.
Serous cavity filariasis is caused by the worms Mansonella perstans and Mansonella ozzardi which occupy the serous cavity of the abdomen.
Causal organisms of Lymphatic filariasis:
Lymphatic filariasis is caused by infection with nematodes (roundworms) of superfamily Filarioidea. There are three types of worms known to cause lymphatic filariasis. These are Wuchereria bancrofti, Brugia malayi and Brugia timori. Wuchereria bancrofti is the most common causal organism of lymphatic filariasis and occurs throughout the world. Brugia malayi is found in South-West India, China, Indonesia, Malaysia, South Korea, Philippines and Vietnam while Brugia timori is only confined to Indonesia. In Wuchereria bancrofti the male worm is 40 mm long while the female is about 50-100 mm long.
Global distribution of Lymphatic filariasis:
Lymphatic filariasis occurs throughout the tropics and sub-tropics of Asia, Africa, the Western Pacific, and parts of the Caribbean and South America. Approximately 65% of those infected live in the South-East Asian region, 30% in the African region and the remaining in other tropical regions of the world.
Lymphatic filariasis and India:
Lymphatic filariasis is a major health problem in India. It is endemic and persistently occurs in the states of Uttar Pradesh, Bihar, Jharkhand, West Bengal, Andhra Pradesh, Odisha, Tamil Nadu, Gujarat, Kerala and Union Territories of Lakshadweep and Andaman and Nicobar islands. Two types of lymphatic filarial infections namely Wuchereria bancrofti and Brugia malayi occur in India. Bancroftian filariasis is responsible for about 98% of the infection in India.
Transmission of Lymphatic filariasis:
Lymphatic filariasis is transmitted by mosquitoes which serve as vectors for the parasitic worms. Humans are the main hosts for the parasite and mosquito is the carrier, an intermediate host. Bancroftian filariasis is transmitted by Culex quinquefasciatus (tropical house mosquito) while the Brugian filariasis is transmitted by Mansonia annulifera, Anopheles barbirostris and Aedes niveus.
Migration of people in search of work from worm-infested areas, urbanization, industrialization, poor housing, ignorance, and inadequate sanitary conditions have led to the transmission of lymphatic filariasis. Generally, about 15,000 to 20,000 bites over several months to years may be required to infect a person. Adult worms freely live in the human lymph system. The lymph system maintains the body’s fluid balance and fights infection. The larvae (microfilariae) circulate in the bloodstream of the infected person. An adult worm may live for about 7 years.
Life cycle of Lymphatic filarial worms:
Human filarial nematode worms have a very complex life cycle, which primarily consists of five stages. After the mating of male and female worms, the female gives birth to thousands of live microfilariae. The microfilariae are taken up by the mosquito (intermediate host) during a blood meal. In the intermediate host (mosquito), the microfilariae molt and develop into third-stage (infective) larvae. Upon taking another blood meal, the mosquito injects the infectious larvae into the dermis layer of the skin. After about one year, the larvae molt through two more stages, maturing into the adult worms.
Symptoms of Lymphatic filariasis:
The incubation period for lymphatic filariasis is not definitely known. However, the disease symptoms appear about 18-16 months after the mosquito bite. Most of the signs and symptoms of lymphatic filariasis are a result of the adult worms invading in the lymph system. Tissue damage caused by the worms restricts the normal flow of lymph fluid. This results in swelling (lymphoedema) scarring and infections. The legs and groin are the most affected part of the body. Lymphatic filarial infection is manifested by a general body weakness, headache, nausea, low-grade fever and recurring attacks of itching.
Lymphatic filariasis is rarely fatal, however, it can cause recurring infections, fevers, severe inflammation of the lymph system and a lung condition called tropical pulmonary eosinophilia. The symptoms of pulmonary eosinophilia include cough, shortness of breath and wheezing. In lymphatic filariasis, the legs become swollen in about 5% of infected persons (this condition is called as elephantiasis). Lymphatic filariasis can lead to severe disfigurement, decreased mobility, and long term disability.
Lymphatic filariasis also causes hydrocele (accumulation of fluid in the scrotum). The patient also may have their testicles swollen, a condition called filarial scrotum. Milky urine is also seen in some patients. In females, breast or external genitals are affected. In some cases, fluid accumulation is found even in the pericardial space (the space between the heart and its thin membrane covering).
Detection of Lymphatic filarisis:
The microfilariae of the parasite can be detected in blood by microscopic examination. The microfilariae had to be detected in blood samples obtained late at night since in most parts of the world the parasites have a ‘nocturnal periodicity’ that restricts their appearance in the blood to the hours around midnight. It has also been discovered that the appearance of parasites in blood is related to the sleep habits of the person. A thick smear of collected blood should be made and stained with Giemsa or Haematoxylin and Eosin. For increased sensitivity, concentration techniques can be used.
Serologic techniques provide an alternative to microscopic detection of microfilariae for the diagnosis of lymphatic filariasis. Patients with active filarial infection typically have increased levels of anti-filarial IgG4 (Immunoglobulin G4) in the blood and these can be detected using routine assays.
Prevention and Control of Lymphatic filariasis:
The number of lymphatic filariasis infected persons is increasing worldwide due to uncontrolled urbanization in areas where the parasite is common. In India occurrence and spread of lymphatic filariasis is a matter of serious concern and needs attention. Since lymphatic filariasis is rarely fatal, hence it is not receiving much attention. If lymphatic filariasis is not treated early enough, the disease leads to severe disability. In the later stages, the amputation of the affected part is only surgical treatment. Long term exposure and repeated infections can cause severe damage to the lymph system and serious complications like gangrene of the foot.
Elephantiasis is common among those who walk barefoot. Therefore, footwear could reduce the risk of infection.
Diethylcarbamazine citrate (DEC) is the drug of choice for controlling the filarial infection. Diethylcarbamazine citrate (DEC) paralyzes the filarial worms. The paralyzed worms are destroyed by the white blood cells of the body. In lymphatic filariasis endemic areas, the regular use of Diethylcarbamazine citrate (DEC) fortified salt can prevent the occurrence of a new infection. Besides DEC, albendazole and ivermectin are the other two anti-filarial drugs which can be used to prevent the occurrence of disease.
Since the disease is transmitted by mosquitoes, hence control of the mosquito populations will avoid the chances of infection. The indoor and outdoor application of insecticides in endemic regions may help to protect human populations from infections.
An aquatic weed Pistia lanceolata favors the breeding of mosquitoes, therefore the weed should be destroyed using the physical, biological or chemical methods of weed control in the rainy season. Biological control agents such as fishes, bugs, meso-cyclops, biolarvicides, and fungi should be used to control the mosquito population.
The two larvivorous fishes namely Gambusia affinis and Poecilia reticulata have been used extensively almost throughout the world for control of mosquito breeding. Fishes such as Aplocheilus blochi, Danio rario, Rasbora daniconius, and Orzias melastigma have good larvivorous potential hence they can also be used to control the mosquito population.
Biolarvicides formulations of Bacillus sphaericus and Bacillus thuringiensis should be used for the control of mosquitoes. The fungi Coelomomyces, Lagenidium and Metarhizium, the nematodes Romanomermis culicivorax and Romanomermis iyengari can be used to control mosquito breeding in aquatic habitats.
Several aquatic insects have been reported as natural enemies of mosquitoes such as water scorpion, water boat, water bug, etc. can also be used to control the mosquito population. An aquatic fern Azolla pinnata has also been reported to control mosquito breeding in paddy fields as it forms a thick layer on the water surface to inhibit oviposition and also act as a bio-fertilizer by fixing elemental nitrogen. Hence Azolla pinnata should be used to curb the mosquito population.
Mosquito nets and mosquito repellent ointments should be used regularly to avoid the mosquito bite.
In the lymphatic filariasis endemic region, one should avoid being bitten by a mosquito by staying indoors between dusk and nightfall. This is the time when mosquitoes are most active. Wearing long pants and long-sleeved shirts also provide protection against mosquito bites.
Conclusion:
It can be concluded that lymphatic filariasis is an infectious disease of body deformities that persists as a serious health problem in tropical and sub-tropical regions of the world. Though the disease is not fatal yet it leads to the disfigurement of the body parts, reduces mobility and causes long term disability. Therefore, prevention and control of lymphatic filariasis is the need of the hour which would be helpful in complete eradication of the disease.
-X-X-X-X-
 Dr. Arvind Singh is M. Sc. and Ph. D. in Botany with an area of specialization in Ecology. He is a dedicated Researcher having more than four dozen published Research Papers in the Journals of National and International repute. His main area of Research is Restoration of Mined Lands. However, he has also conducted research on the Vascular Flora of Banaras Hindu University-Main Campus, India.
Dr. Arvind Singh is M. Sc. and Ph. D. in Botany with an area of specialization in Ecology. He is a dedicated Researcher having more than four dozen published Research Papers in the Journals of National and International repute. His main area of Research is Restoration of Mined Lands. However, he has also conducted research on the Vascular Flora of Banaras Hindu University-Main Campus, India.
keywords: lymphatic filariasis symptoms, lymphatic filariasis pictures, lymphatic filariasis treatment, lymphatic filariasis life cycle, lymphatic filariasis history, lymphatic filariasis diagnosis, lymphatic filariasis prognosis, lymphatic filariasis spread, lymphatic filariasis india, towards elimination of lymphatic filariasis in india, economic burden lymphatic filariasis in india, lymphatic filariasis in india epidemiology control measures, lymphatic filariasis elephantiasis, lymphatic filariasis national, lymphatic filariasis development, status of lymphatic filariasis, filariasis treatment in india, lymphatic filariasis prevention